Email
info@lgsc.co.uk
Email
info@lgsc.co.uk
Phone
0203 312 6130
Location
The Lindo Wing, St Mary’s Hospital,
Praed Street, London W2 1NY
Gallstones occur when bile, which is normally fluid, forms stones. Gallstones commonly contain lumps of fatty (cholesterol-like) material that has solidified and hardened. Sometimes bile pigments or calcium deposits form gallstones. They vary in number and size. About one in three women, and one in six men, form gallstones at some stage in their life. Gallstones become more common with increasing age. The risk of forming gallstones increases with pregnancy, smoking, obesity, rapid weight loss, having a close relative with gallstones, diabetes and certain medicines such as the contraceptive pill.
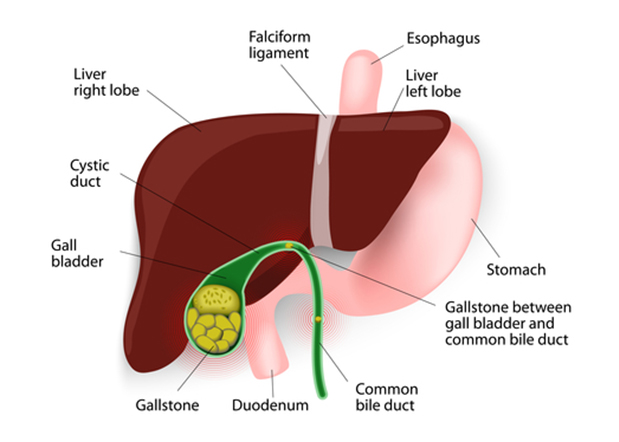
Bile is a fluid made in the liver. Bile contains various substances including bile pigments, bile salts, cholesterol and lecithin. Bile is passed into tiny tubes called bile ducts. The bile ducts join together (like the branches of a tree) to form the main bile duct. Bile constantly drips down the bile ducts, into the main bile duct, and then into the initial part of small bowel (small intestine). It helps to digest food, particularly fatty foods. The gallbladder lies under the liver on the right side of the upper abdomen. It is like a pouch, which is connecting to main bile duct with a small tube, cystic duct. It is a ‘reservoir’ that stores bile. The gallbladder squeezes (contracts) when we eat. This empties the stored bile back into the main bile duct.
Most people with gallstones do not have any symptoms or problems, and do not know they have them. Commonly, the stones simply stay in the gallbladder and cause no harm. However, about one out of three people with gallstones develop symptoms.
This is a severe pain in the upper abdomen. The pain is usually worst to the right-hand side, just below the ribs because a stone gets stuck in the cystic duct, a small tube that connects gallbladder to the main bile duct causes it. The gallbladder then squeezes (contracts) hard to dislodge the stone, and this causes pain. The pain eases and goes if the gallstone is pushed out into the bile duct (and then usually out into the intestine), or if it falls back into the gallbladder.
Pain from biliary colic can last just a few minutes but more commonly, lasts for several hours. A severe pain may only happen once in your lifetime, or it may flare up from time to time. Sometimes less severe but niggly pains occur now and then, particularly after a fatty meal when the gallbladder contracts most.
Ultrasound scan and blood tests are the most common investigations done. Other investigations including different types of scans may sometimes be required. Once gallstones start giving symptoms, surgery is the best treatment. In patients where there is a high risk of forming stones again in the main bile duct, medicine to dissolve small stones may be given to prevent gallstones from developing.
It is the inflammation of the gallbladder. In majority of cases, cholecystitis is thought to be caused by gallstones. What seems to happen is that a gallstone becomes stuck in the cystic duct (this is the tube that drains bile out from the gallbladder into the bile duct). Bile then builds up in the gallbladder, which becomes stretched (distended). Because of this, the walls of the gallbladder become inflamed. In some cases the inflamed gallbladder becomes infected. An infected gallbladder is more prone to lead to complications.
Symptoms usually develop quickly and include abdominal pain, raised temperature, and being generally unwell. In some cases, jaundice may result when gallstones get stuck in the bile duct. Bile then cannot pass into the gut, and so seeps into the bloodstream. This causes the patient to become yellow (jaundiced).
The stone may eventually be passed into the gut. However, it is common to need a procedure to remove a gallstone, which has become stuck in the bile duct.
Complications of cholecystitis include progression to severe infection, decay of gallbladder tissue (become gangrenous), blood poisoning (septicaemia), gallbladder bursting (perforation) and a channel (fistula) forming between the gallbladder and gut as a result of continued inflammation. All these complications are very serious and can be life-threatening.
An ultrasound scan is commonly done to clarify the diagnosis. This is a painless test, which uses sound waves to scan the abdomen. An ultrasound scan can usually detect gallstones, and assess for gallbladder inflammation. If the diagnosis is in doubt then other more detailed scans may be done.
Management of cholecystitis requires hospital admission. To rest the gallbladder, patient is not allowed to eat or drink for first 24-48 hours. Fluids, painkillers and antibiotics are given directly into a vein through a 'drip'. With this initial treatment the gallstone that caused the blockage often falls back into the gallbladder, and the inflammation and symptoms often settle down. Surgery is a definite treatment for cholecystitis caused by gallstones. It is performed once the infection settles down - usually a few weeks later. Keyhole surgery, laparoscopic cholecystectomy, is now the most common way to remove a gallbladder.
If you do not have your gallbladder removed, there is a reasonable chance that you will have no further problems if the inflammation settles down. However, there is also a good chance that you would have further bouts of cholecystitis in the future. This is why the usual treatment is to remove the gallbladder.
After the operation, there is no impact on the body’s ability to digest food. Bile still flows from the liver to the gut once the gallbladder is removed. You can usually eat a normal diet without any problems. However, up to half of people who have had their gallbladder removed can have some mild abdominal pain or bloating from time to time. This may be more noticeable after eating a fatty meal. Some people notice an increase in the frequency of passing stools (motions, or faeces) after their gallbladder is removed. This is like mild diarrhoea. It can be treated by antidiarrhoeal medication if it becomes troublesome.

Please note, most insurance policies in the UK do not cover weight-loss surgery. However, we will do our utmost to provide the best package for you should you choose to have your surgery with us.
The contents on this site is for information only, and is not meant to substitute the advice of your own physician or other medical professional.