Email
info@lgsc.co.uk
Email
info@lgsc.co.uk
Phone
0203 312 6130
Location
The Lindo Wing, St Mary’s Hospital,
Praed Street, London W2 1NY
A diverticulum is a small pouch with a narrow neck that sticks out from the wall of the bowel (intestine). Diverticula mean more than one diverticulum. They can develop on any part of the bowel, but usually occur in the left sided large bowel (large intestine) towards back passage (rectum). They become more common with increasing age. About half of all people in the UK have diverticula by the time they are 50 years old. Nearly 7 in 10 people have diverticula by the time they are 80 years old.
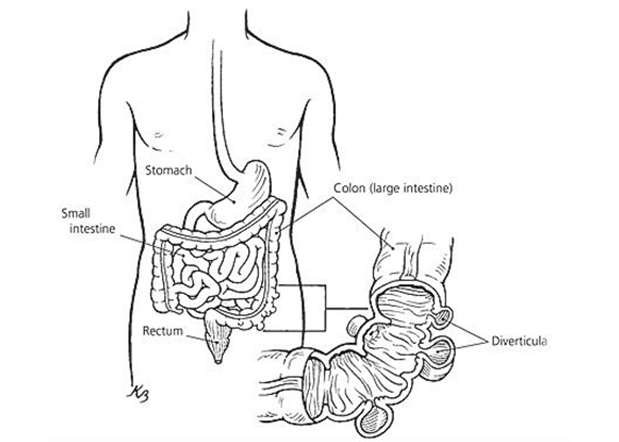
The reason why diverticula develop is related to not eating enough fibre. Fibre is the part of food that is not digested but is very helpful for bowel muscles to move the faeces. If there is too little fibre, the bowel muscles have to work harder to push faeces resulting in high-pressure regions developing within bowel pushing the inner lining of a small area of the gut through the muscle wall to form a small diverticulum.
In about 3 out of 4 people who develop diverticula, the diverticula cause no harm or symptoms, defined as diverticulosis. The term, diverticular disease, is used when diverticula cause intermittent, crampy, lower abdominal pain or bloating. Since most of the diverticula develop in the left sided large bowel (colon), patient experiences pain on the left lower side of abdomen. Some people develop diarrhoea or constipation, and some people pass mucus with their stools. A diverticulum may occasionally bleed and you may pass some blood via your back passage. The bleeding is usually abrupt and painless. The bleeding is due to a burst blood vessel that sometimes occurs in the wall of a diverticulum. A very large bleed may occur in some cases requiring an emergency blood transfusion. In rare cases, an operation is needed to stop the bleeding. Diverticular disease is diagnosed by colonoscopy test, a special flexible telescope to look into the bowel. This can confirm the presence of diverticula. It also rule out bowel cancer, which may present similarly to diverticular disease in elderly patient.
The management of the condition includes:
A high-fibre diet is usually advised as it helps to keep stools (faeces) soft and bulky and reduces pressure on the colon, which should come from a variety of high-fibre foods.
Increased fluid intake, aim to drink at least two litres per day of water.
Paracetamol can ease pain if a high-fibre diet or fibre supplements do not help so much to ease pain. Other types of painkiller are not usually used for diverticular disease and try to avoid anti-inflammatory painkillers such as aspirin, diclofenac, ibuprofen, and naproxen.
Diverticulitis is a condition where one or more of the diverticula become inflamed and infected. This may occur if some faeces get trapped and stagnate in a diverticulum. Germs (bacteria) in the trapped faeces may then multiply and cause infection. About 1 in 5 people with diverticula develop a bout of diverticulitis at some stage. Some people have recurring bouts of diverticulitis. Symptoms of diverticulitis include lower abdominal pain associated with fever, diarrhoea or constipation, blood in stool and sickness (nausea/vomit). Diverticulitis can lead to the following complications: obstruction (blockage of large bowel), abscess (collection of pus), fistula (an abnormal channel between two organs), perforation (hole in the bowel). Surgery is usually needed to treat these serious but uncommon complications.
When patient with acute severe pain is suspected of the condition, blood tests are carried out and usually CT scan is conducted to confirm diagnosis. The management of diverticulitis needs a course of antibiotics and plenty of clear fluids. During acute infection, it is adviced to take pain killers (preferably paracetamol), drink only fluids followed by soft diet as the symptoms settle. Once symptoms resolve, you can resume a normal diet or a high-fibre diet is usually best. If symptoms are severe, hospital admission is required to give antibiotics and fluids directly into a vein via a drip as well as injections of painkillers. You may also be admitted to hospital if the symptoms are not too severe but do not settle after 48 hours or so with antibiotic tablets.
Please note that a sudden change from your normal bowel habit to persisting constipation or diarrhoea, passing blood or mucus, or new pains require a review from a doctor even if you are known to have diverticula because a change of symptoms may indicate a new and different intestinal problem and it is important to exclude bowel cancer. Call an ambulance urgently if you have a large amount of bleeding from the bowel.

Please note, most insurance policies in the UK do not cover weight-loss surgery. However, we will do our utmost to provide the best package for you should you choose to have your surgery with us.
The contents on this site is for information only, and is not meant to substitute the advice of your own physician or other medical professional.